Historically, the need for education and services to improve healthcare in Haiti has been overshadowed by a lack of valuable resources; resources depleted through a string of political struggles and natural disasters. The earthquake of January 12th 2010 crippled the healthcare system of a country that was already on its knees. To the large percentage of pre-existing disability in Haiti, the earthquake delivered an additional estimated 4-6,000 amputee, countless crush injuries, spinal cord injuries and burns. All required intensive rehabilitation.
The science based practice of Physiotherapy uses a physical approach of rehabilitation to promote restoration and maintenance of physical function. Haiti has no national education program for Physiotherapy, and only a handful of Haitian Physiotherapists (PT`S) trained by overseas staff, so there is a limited understanding of the possibilities of rehabilitation practices. In the wake of the earthquake, it was hard to imagine how the overwhelming surge of disability would be managed. Subsequently, the challenges of creating functional and sustainable rehabilitation services in Haiti would not only become a logistical nightmare, but also one requiring understanding and adaptation to cultural and environmental factors.
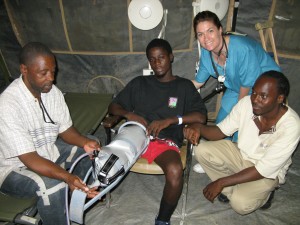 The Initial Response
The Initial Response
During the initial response to this phenomenal disaster, hospitals were overwhelmed by the sheer number of patients flooding through their doors. Concern was being raised over the lack of Physiotherapists (PT`s) despite NGO`s trying to meet the level of unmet need. PTs were essential to reduce hospital length of stay by enhancing recovery from illness and physical disability. However, the few PT`s in the country were struggling to deal with the many secondary complications that arose due to prolonged inactivity and bed rest. Lives were being lost because of the lack of prompt treatment. Lethal pressure sores, sepsis, respiratory failure and deep vein thrombosis presented rapidly in many patients.
These complications are not only manageable but preventable with early diagnosis and intervention such as mobilization, exercise and education. Despite attempts to prioritize high risk patients, with limited numbers of PT`s, intervention remained a challenge.
Hôpital Sacré Coeur Takes On the Challenge
In rising to the challenge of providing physiotherapy services, Hôpital Sacré Coeur (HSC) was able to coordinate a constant supply of PT`s and PT Techs, mostly from the States, on weekly rotations. As a PT and Coordinator of Rehab Services at the HSC, I felt blessed to receive each week’s supply of highly skilled therapists. Not only were they all eager to get to work helping the 450 quake victims who resided in our tents, they also bought greatly needed supplies. Even so, at times we still lacked equipment such as braces and walking aids. We found creative ways to meet the need.
 Equipment to strengthen and mobilize muscles and joints were hand made out of local materials. We made hand weights out of bandages and bottles filled with sand and rocks. Wobble boards for exercising ankles and knees were made out of cannon balls from a local ancient monument. Parallel bars were welded by local craftsmen, a small boost to local enterprise! We were extremely fortunate when a volunteer arrived with a PPAM aid, a specialized piece of equipment for preparing amputees to walk with limbs. A therapy patio was made outside the tents to facilitate group work and classes, including dance parties, a fun way for our patients’ to reclaim social interaction.
Equipment to strengthen and mobilize muscles and joints were hand made out of local materials. We made hand weights out of bandages and bottles filled with sand and rocks. Wobble boards for exercising ankles and knees were made out of cannon balls from a local ancient monument. Parallel bars were welded by local craftsmen, a small boost to local enterprise! We were extremely fortunate when a volunteer arrived with a PPAM aid, a specialized piece of equipment for preparing amputees to walk with limbs. A therapy patio was made outside the tents to facilitate group work and classes, including dance parties, a fun way for our patients’ to reclaim social interaction.
Translation was provided for those with no knowledge of Creole or French. However, deciphering foreign notes for patients arriving from field hospitals run by Russians, Italians and other foreign nations responding to the quake, would always prove difficult.
Given the physical nature of Physiotherapy, the extreme heat would also be challenging. Temperatures in the tents would soar over 100 degrees, requiring a different pace of work and constant refreshment to avoid time on the staff sofa having bags of Intra-Venous fluids. The emotional fatigue of working within an environment with so many people suffering from great pain, disability and loss was something less easily avoided. It can be hard to maintain the professional boundaries of first world medicine and reduce the emotional attachment that naturally arises when you are practicing in third world. In first world medicine, we rarely find our patients or their families offering to braid our hair, sing or pray with us when they’re in pain or that they expect the whiteness of our skin to perform some kind of miracle for them.
At times, the weekly rotations of staff took their toll. No sooner would a PT get to know the patients and their specific abilities and needs, then the PT would have to leave, and so it would continue week after week. As a result, the arrival of PT`s committed to long term rotations was particularly beneficial and brought great advantage to our patients and therapy staff themselves.
 We were also fortunate to have an electronic patient data system to remove some of the challenges seen in the constant handover of information. This provided much needed continuity and consistency of care. However, this would still be difficult for certain patients who had come from many different areas of Haiti. At some point they would be discharged home. We were concerned about how they would obtain the long term assistance required.
We were also fortunate to have an electronic patient data system to remove some of the challenges seen in the constant handover of information. This provided much needed continuity and consistency of care. However, this would still be difficult for certain patients who had come from many different areas of Haiti. At some point they would be discharged home. We were concerned about how they would obtain the long term assistance required.
Meeting the Special Needs of Patients
Amputees and those with Spinal Cord Injury (SCI) are highly vulnerable and face long term disability. They also have a high risk of mortality from secondary complications. We were blessed with the arrival of a prosthetics lab to make new limbs and with hospital facilities in which to perform lifesaving spinal surgery. As a result, many people received new limbs and recovered the use of ones that had once been paralyzed.
Some of these patients however would need specialist care and physiotherapy for many years to come. To maintain functional ability, amputees would require new prosthetics as they grew, especially the children, and SCI patients would need long term care to avoid secondary complications. Whilst educating family members in specialized knowledge and skills would help, for those who still had family, our concerns for ongoing professional support were rising.
 The Challenges of Providing Long Term Care
The Challenges of Providing Long Term Care
Difficulties in continuity of care and national coordination were being felt all over Haiti due to poor infrastructure and communication between services. However, The Injury, Rehabilitation and Disability Working Group (IRD), initiated by the UN, would ease such problems. This group works with the assistance of the Haitian government`s Ministry of Public Health and Population (MSPP) and Secretariat for the Integration of People with Disabilities (SEIPH), and is a major component of Haiti’s National Reconstruction Plan. With the IRD facilitating national rehabilitation efforts and communication across Haiti, everyone working within the Haitian health sector could share resources and gain access to valuable information and assistance.
NGO rehabilitation specialists such as Handicap International and Healing Hands for Haiti are key players of the IRD. Their knowledge, stemming from many years’ experience of working in Haiti, was of great value in facilitating physiotherapy services due to their in-depth understanding of cultural and environmental factors. This made them ideally placed to set up accessible physiotherapy stations with outreach services to local communities; communities which had now become tent cities. Community based rehabilitation (CBR) has become a vital and sustainable source of physiotherapy, bringing support and adaption to the progressive and, for amputees and SCI patients, long term need. Although with minimal knowledge of Physiotherapy, many Haitians, including healthcare professionals, have little understanding of the possibilities of rehabilitation.
Hôpital Sacré Coeur Provides Training for Haitian PT Techs
Within the walls of first world hospitals patients benefit from specialized, multidisciplinary healthcare. However, within the walls or tents of third world hospitals such as Haiti, healthcare can be seen as a skeleton of such privileged services where opportunities for specialist care rely heavily on overseas assistance. Thus, the training of Haitian PT`s has become a major part in improving healthcare and reducing disability in Haiti. At HSC, our teams of PT`s were complemented by having two Haitian PT Techs who were keen to assist and learn new knowledge and skills. They were also a bridge in allowing us to improve understanding of rehabilitation, not only for our patients, but also other members of Haitian staff who had little experience or knowledge of our roles.
 Poor understanding of the methods and goals of Physiotherapy could generate difficulties even when dealing with patients. A typical example concerned progressing weight bearing when we would try to take back walking aids in order to advance our patients’ gait and mobility. Patients were very reluctant to give back their nice shiny crutches or walking sticks. We were, it would seem, reclaiming gifts we had given people who had lost everything in the quake. Many times I would smile when finding a wealth of therapy aids and devises under a patient’s bed, thinking how well placed they would be to start their own CBR once they got home……maybe this wasn’t a bad thing at all!
Poor understanding of the methods and goals of Physiotherapy could generate difficulties even when dealing with patients. A typical example concerned progressing weight bearing when we would try to take back walking aids in order to advance our patients’ gait and mobility. Patients were very reluctant to give back their nice shiny crutches or walking sticks. We were, it would seem, reclaiming gifts we had given people who had lost everything in the quake. Many times I would smile when finding a wealth of therapy aids and devises under a patient’s bed, thinking how well placed they would be to start their own CBR once they got home……maybe this wasn’t a bad thing at all!
Many Haitians` understanding of illness and disability can be very different to that of the first world. Whilst poor education can account for some of this, cultural differences would also need to be embraced. This would allow us to improve compliance with treatments and, ultimately, facilitate multidisciplinary healthcare with a sustainable workforce of Haitian PT`S.
Common Haitian Perceptions about Disability
The concept of disability in Haiti can carry connotations that are both mysterious and dangerous such as the belief that a curse or punishment has been placed upon someone from either another person or even God. As such, disability has often been seen as something shameful leading to exclusion from society. With improved education and awareness of underlying pathophysiology, a more realistic awareness of disability can be possible. It has also been thought that with such a great rise of disability since the quake, Haitian society has been altered. As disability has now become more ‘normal’ in a sense, many will gain empowerment from each other and feel less likely to be excluded.
Greater understanding of the need to perform exercise can also reduce the typically held belief that “I will get out of bed or move when I feel better”. In adopting this sick role, many Haitians require the knowledge that muscles and joints will move easier and with less pain when allowed to heal through progressive loading and movement. Whilst family support is admirable in Haiti, it also reduces important activity due to family members inadvertently doing everything for those with disabilities, reducing the promotion of independence and functional ability.
By embracing an understanding of cultural values and attitudes to disability, Physiotherapists are uniquely placed to alter the futures of many Haitians. We are therefore in a prime position to help lift Haiti back onto its feet.
 Joanna Woodrow, P.T. is a UK qualified and registered Physiotherapist who spent 6 months working in Haiti as a medical volunteer. She served as the Rehabilitation Coordinator for Hôpital Sacré Coeur and also helped set up a Spinal Cord Injury network in Haiti. Joanna is very passionate about humanitarian needs and sustainable healthcare in third worlds. Her particular interest and sensitivity to the needs of patients with spinal cord injuries developed after her father was paralyzed in a car crash four years ago.
Joanna Woodrow, P.T. is a UK qualified and registered Physiotherapist who spent 6 months working in Haiti as a medical volunteer. She served as the Rehabilitation Coordinator for Hôpital Sacré Coeur and also helped set up a Spinal Cord Injury network in Haiti. Joanna is very passionate about humanitarian needs and sustainable healthcare in third worlds. Her particular interest and sensitivity to the needs of patients with spinal cord injuries developed after her father was paralyzed in a car crash four years ago.