 By Harold Prévil, M.D., CEO Hôpital Sacré Coeur
By Harold Prévil, M.D., CEO Hôpital Sacré Coeur
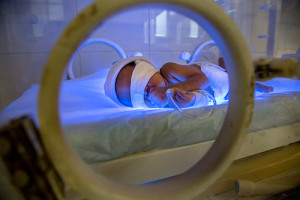
This sounds like the headline of a newspaper; but no, this is the reality at Hopitâl Sacré Coeur of Milot: a reality that needs to change and to change fast. One simple question that could be asked of us is, “Why does a center like ours agree on such inadequate accommodation?” I would simply reply: this is a matter of life or death for this newborn. We are aware of the cross infection’s risk, but beyond this risk, we are pretty sure about the outcome if we said “No” to the mother or the father of this premature baby, who was born at the hospital or referred to us by another facility. Without this less than desirable attempt, the baby would most likely die.

HSC Pediatrician Dr. Exavier tends to one of his NICU patients
Do we have a solution to this problem? Our answer is “Yes.”
In 2000, 189 UN member nations developed the Millennium Declaration Goals, a set of shared values for improving human health. Goal #4 is to reduce child mortality and Goal #5 is to improve maternal health. In 2013, Aye Otubu, MD of Howard University Hospital teamed with Ha-young Choi, MD and Deborah Hoy, MD of MedStar Georgetown University Hospital to access neonatal survival rates at Hopitâl Sacré Coeur in Milot, Haiti.
The clinical research team reviewed the available HSC maternity register which covered 12 months of deliveries (4/30/13 – 4/30/14 and compared to 10 months of data 5/1/14 – 3/10/15), identified all recorded newborn deaths, and pulled data on GA, sex, DOB, complications, delivery mode, wt, apgars, and prenatal care. Findings showed neonatal death rates well below the WHO average rates for developed countries and significantly above the Haiti national neonatal death rate of 25 per 1000 live births.
From April 2013 – April 2014, HSC recorded 1107 total births with 57 deaths (57 per 1000 live births) and more specifically 41 neonatal deaths per 1000 live births (first 24 hours). From May 2014 – March 2015, HSC recorded 1130 total births in 10 months with 63 deaths (56 per 1000 live births) including 35 neonatal deaths per 1000 live births (first 24 hours). There was approximately equal number of male and female infants in both years.
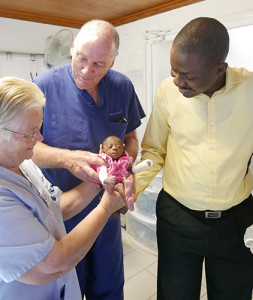
Dr. Prévil joins Sr. Ann Crawley and Dr. David Butler in welcoming a newborn.
Data analysis concluded that simple interventions targeting term and moderate to late pre term (32 > 37 weeks) could significantly decrease the rate of neonatal deaths. In order to accomplish this goal, the medical research team recommended: 1. Have a nurse trained in “Helping Babies Breathe” protocols available for every delivery, 2. Develop and implement medically and culturally appropriate strategies to increase rate of prenatal care and identification of high-risk pregnancy, 3. Establish quality measures to monitor over the next year in tandem with accurate data collection; and 4. Institute a hand washing campaign encompassing before and after care.
To support these goals and continue to improve the care we are providing to the newborns and the children, our hospital is looking for financial support to build a new pediatric wing.
We want, through this project, to double the size of our neo-natal intensive care unit or NICU, moving from ten bassinets to twenty. We will also add 20 more cribs for bigger children, an isolation wing for children with infectious disease; and, we will also develop a playground — an environment that will help the children recover faster.

Sr. Ann watches over two infants in the same bassinet
God bless you all.
Harold Prévil, M.D.
CEO, Hôpital Sacré Coeur









