 By M.K. Resk
By M.K. Resk
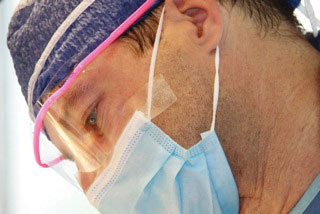
Wandering around Milot with Dr. Jeff Monda is like walking with a celebrity. The urologist from Washington state has been coming to Haiti once, twice, or sometimes three times a year since 2007. Vendors, locals, and former patients alike recognize and appreciate the great work Dr. Monda and his team provides.
Dr. Monda started coming to Haiti because of a few colleagues with a long history at CRUDEM, urologist Dr. Dale Peterson and certified urology technician, Fred Schuenemann.
Now retired, Dr. Peterson was instrumental in CRUDEM’s leadership for a number of years starting in 1998. Schuenemann recalls that Dr. Peterson became a Knight of Malta to become a CRUDEM board member. Schuenemann started accompanying Dr. Peterson in order to set up endoscopic surgery in Milot. He was instrumental in getting supplies to Haiti and developing a functional system for endoscopic work. He now assists Dr. Monda and fellow Wenatchee, WA urologist, Dr. Wally Gibbons, on their trips to Haiti.
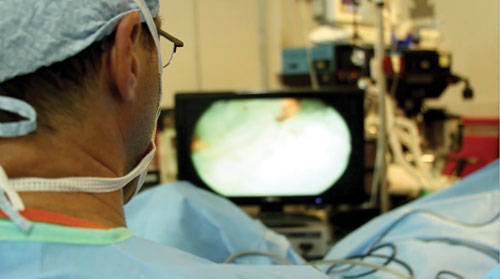 “People like Dale Peterson pioneered down there ahead of us, laid the groundwork and made it easy. And people like Fred Schuenemann provide an amazing amount of work for us to be able to do what we do without the stress of day-to-day set up,” Dr. Monda acknowledges.
“People like Dale Peterson pioneered down there ahead of us, laid the groundwork and made it easy. And people like Fred Schuenemann provide an amazing amount of work for us to be able to do what we do without the stress of day-to-day set up,” Dr. Monda acknowledges.
Dr. Monda says patient evaluation, treatment, and recovery in Haiti are in some ways identical to his practice in the United States. The biggest differences in Haiti are severity of problems and limited diagnostics. “You can’t get CAT scans, you have to make do with less,” Dr. Monda says.
But he says he still gathers all of the information he needs and makes the right decisions for his patients, never compromising quality of care.
 Many Haitian urology patients present similarly to U.S. patients, but Dr. Monda sees more people with urgent symptoms in Haiti. For instance, whereas in the U.S. he might see a handful of people a month with urinary retention (keeping them from urinating), in Haiti a significant number of the 100 patients he’ll see within a 5-6 hour clinic are in retention. He also sees diseases that are specific to Haiti, such as a microfilarial worm that causes elephantiasis, a big swelling of the testicles. “We see some swelling of the testicles, hydroceals in the U.S. but nothing compared to what you see in Haiti,” he says.
Many Haitian urology patients present similarly to U.S. patients, but Dr. Monda sees more people with urgent symptoms in Haiti. For instance, whereas in the U.S. he might see a handful of people a month with urinary retention (keeping them from urinating), in Haiti a significant number of the 100 patients he’ll see within a 5-6 hour clinic are in retention. He also sees diseases that are specific to Haiti, such as a microfilarial worm that causes elephantiasis, a big swelling of the testicles. “We see some swelling of the testicles, hydroceals in the U.S. but nothing compared to what you see in Haiti,” he says.
Because his Haitian patients’ prostate and urinary problems are often so apparent, Dr. Monda finds that many times he doesn’t need the same diagnostic tests as he would back home. “In Haiti they may have had a catheter in for five years, so it may become very, very clear what their problem is. Their prostates are very big, their testicles are very big, their hydroceals are very big,” he says. “You’re dealing with a lot of basic care that only urologists can provide.”
Dr. Monda calls urology a very technology-based field. Because of this, diagnostic and treatment options are restricted in Haiti. For example, kidney stones are especially difficult to diagnose and treat there, he says.
Consequently, treating kidney stones in Haiti is like treatment in the U.S. was forty or fifty years ago.
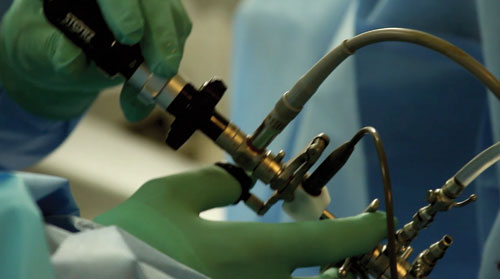 Yet Dr. Monda and his team have been able to adapt modern technical procedures and equipment for use in the conditions they find in Haiti. High quality equipment now enables them to perform surgical procedures for enlarged prostates–transurethral resection of the prostate (TURPs) — as they are done at home.
Yet Dr. Monda and his team have been able to adapt modern technical procedures and equipment for use in the conditions they find in Haiti. High quality equipment now enables them to perform surgical procedures for enlarged prostates–transurethral resection of the prostate (TURPs) — as they are done at home.
But to do this procedure, they have also had to do a lot of jerry-rigging to create low-tech solutions that emulate the ready-made tools they have available back home.
Accomplishing their tasks takes a lot of planning and thought. Additionally, it requires skills and knowledge that for many medical professionals are a lost art. Dr. Monda credits Fred Schuenemann with organizing and creating many effective devices over the years.
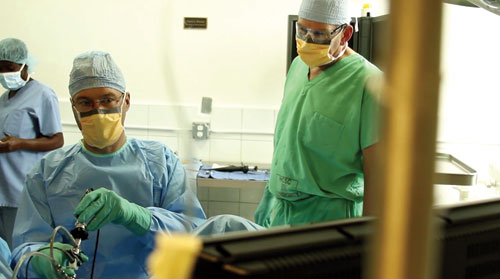 Having worked in the urology field for many years helps, Schuenemann says, “Most people in medicine today can’t imagine or remember what it was like to process your own fluids (sterile saline or sterile water). For me and (Dr. Dale) Peterson it was no big step to mix up our own endoscopic solution.”
Having worked in the urology field for many years helps, Schuenemann says, “Most people in medicine today can’t imagine or remember what it was like to process your own fluids (sterile saline or sterile water). For me and (Dr. Dale) Peterson it was no big step to mix up our own endoscopic solution.”
Besides processing fluids, Schuenemann has developed a system to keep the fluids flowing to the operating table, and he even rigged camera, camera box, and monitor systems together to keep the urologists’ eyes away from any squirts when viewing bladders (and therefore reducing HIV risk-exposure).
Another example of old medical techniques helping new ones came on Dr. Monda’s first trip to Haiti. His father, Dr. George Monda, who had also practiced urology but had been retired for several years, accompanied him.
“There was a patient that had a prostatic urethral disruption, where the urethra breaks away from the prostate,” Dr. Jeff Monda recalls. “He was 19 years old. He had been managed with a suprapubic tube in his bladder for several years,” the younger Dr. Monda remembers. “The only hope was to do a primary repair on that which I had not done in practice. My dad, who had been retired for several years, had done them a lot in his practice, so he was able to guide me through the surgery and fix the problem.”
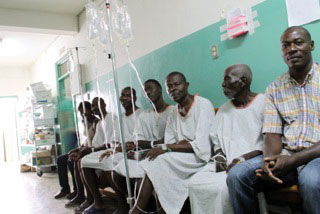 Dr. Monda is also impressed with the improvising that his Haitian patients do. Often he’ll see patients who have had their catheters in for several years but manage just fine in their daily lives. They are “otherwise healthy people who are out there working the fields, doing what they’d be doing normally except they have a catheter in,” he says. “They use makeshift things like plugging their catheters with sticks so their urine’s not leaking out of them all the time. Generally speaking they do very, very well with survivals.“
Dr. Monda is also impressed with the improvising that his Haitian patients do. Often he’ll see patients who have had their catheters in for several years but manage just fine in their daily lives. They are “otherwise healthy people who are out there working the fields, doing what they’d be doing normally except they have a catheter in,” he says. “They use makeshift things like plugging their catheters with sticks so their urine’s not leaking out of them all the time. Generally speaking they do very, very well with survivals.“
Some of those patients travel a long way to get to Hôpital Sacré Coeur, Dr. Monda points out. “Then they sit on the benches all day waiting to be seen. They’re very, very patient. Nobody complains,” he says.
Patients requiring urological follow-up care will sometimes be seen by a general surgeon or can always be seen by the next urologist coming down.
Dr. Monda says there are currently three urologists that visit Milot, staggered relatively evenly throughout the year. Coincidentally, one of them, Dr. Les Rainwater, trained at the Mayo Clinic with Dr. Monda and served as chief resident.
Sometimes the scope of urological problems in Haiti is beyond the ability to care for in remote conditions.
“I’m always amazed in clinic that you’ll see 100 patients in a day and you’ll see patient after patient with common urologic problems. Then you’ll see a baby that’s been born with exstrophy, where the bladder’s open to the outside environment,” Dr. Monda says. “In the U.S. that would be something that would require multiple surgeries and you just don’t have that available in Haiti,” he adds.
In those instances, sometimes a specialist can come to Haiti to provide care. Occasionally a patient will be sent for care in the U.S., but visas and international healthcare can prove very difficult. For these complicated cases, “you’re looking at a lifetime of issues for that patient. You feel very helpless for what you can do in that situation,” Dr. Monda acknowledges.
Not being able to meet the needs of all in Haiti certainly weighs on Dr. Monda’s heart. Why does he continue to go? How has his time in Haiti impacted him?
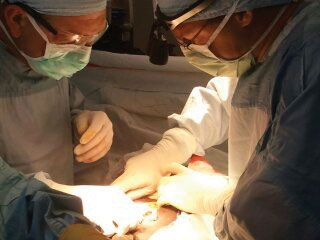 “The whole point of going is to teach. It’s critical to note that we could not do what we do without the welcoming environment of the Haitians who are very well-educated, who have been through thick and thin with the earthquake and who allow us to come in and work with them and teach us a lot. In doing so, they learn a lot from us as well. We feel like guests when we’re there,” says Dr. Monda.
“The whole point of going is to teach. It’s critical to note that we could not do what we do without the welcoming environment of the Haitians who are very well-educated, who have been through thick and thin with the earthquake and who allow us to come in and work with them and teach us a lot. In doing so, they learn a lot from us as well. We feel like guests when we’re there,” says Dr. Monda.
Anesthesiologist Dr. Dave Wiggum has accompanied the Wenatchee urology team several times over the past few years. He says, “It’s fun to work together in the operating room with the Haitian staff and our own staff,” and echoes the teaching goal statement.
Though the language barrier can be difficult to overcome, Dr. Wiggum has enjoyed developing working relationships over the years with the local staff. “Sharing techniques, collaboration with students, CRNAs (Certified Registered Nurse Anesthetists) and operating staff—when that goes well and you feel like you’ve taught someone something or shared something, that can be the best part of the whole thing,” Dr. Wiggum states.
On his most recent visit in April, Haitian CRNA Masiane Jean Baptiste “really wanted to be involved in pediatric urology cases” and Dr. Wiggum was eager to help her build her skills. The Wenatchee team is the only visiting team that performs pediatric urology cases.
Every year the crew joining the Wenatchee, WA team grows. Medical and non-medical community members including a Rotary group have accompanied the Wenatchee contingency. “It’s become a much more community-wide interest that’s not just us who have opened people’s eyes to what’s going on there.
Orthopedics has gone down there twice and have a continued interest in going with us. They started going down after the earthquake and we take down a team that includes usually two anesthesiologists, two urologists, and recovery room nurses, OR nurses, and surgical techs.
When we take orthopedics down we take a complement to handle them as well,” Dr. Monda says.
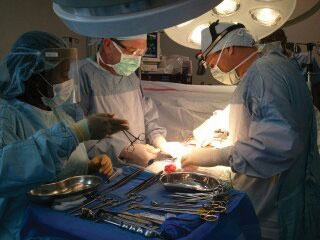 Trips to Haiti have even become a family affair. In addition to his father, Dr. Monda has brought his wife, son, daughters, nieces, brother-in-law, and countless friends along. In a twist of coincidence, a cousin currently operates a nearby children’s home, and another relative has served as a long-term volunteer in Cap Haïtien. “It’s been wonderful to bring family members to see the area and get involved in other concerns there,” says Dr. Monda.
Trips to Haiti have even become a family affair. In addition to his father, Dr. Monda has brought his wife, son, daughters, nieces, brother-in-law, and countless friends along. In a twist of coincidence, a cousin currently operates a nearby children’s home, and another relative has served as a long-term volunteer in Cap Haïtien. “It’s been wonderful to bring family members to see the area and get involved in other concerns there,” says Dr. Monda.
Urology tech Schuenemann is game to continue going to Haiti “for as long as Dr. Monda and Dr. Gibbons and whoever else goes down needs help.” He says Dr. Monda has been absolutely wonderful with a great grasp of life on Haiti and constantly brings things back to reality with humorous questions.
“He’s been a real bedrock of reality to work with,” says Schuenemann. “It’s a meaningful situation and it’s just fun,” he says.
“When we get down there we have an opportunity to take care of people who have serious problems,” says anesthesiologist Dr. Wiggum. “The clinic doctors and CRUDEM staff do a nice job of getting patients pre-screened, lined up, and ready to be seen and evaluated. As a group we have fun and enjoy what we’re doing—meeting and caring for patients,” he adds.
 Dr. Monda sums up his reasons for traveling to Haiti: “Going down to Haiti keeps me interested in continuing in medicine. The day-to-day stresses that happen in medicine in the U.S. make you think you may not like what you’re doing. Then you go down to Haiti and you operate on more people and have less stress.
Dr. Monda sums up his reasons for traveling to Haiti: “Going down to Haiti keeps me interested in continuing in medicine. The day-to-day stresses that happen in medicine in the U.S. make you think you may not like what you’re doing. Then you go down to Haiti and you operate on more people and have less stress.
You realize that it’s not the patient care that causes you stress; it’s everything else. Going to Haiti has made me reflect on the fact that I’d like to stay in medicine longer. I just need to make sure to reflect on what’s important in medicine. It’s helped me ground myself with regard to what’s important in what we do.”
Dr. Jeff Monda received a B.S. from Washington State University and an M.D. from University of Washington School of Medicine. He completed his internship and residency at Mayo Graduate School of Medicine. Dr. Monda is board-certified in Urology by the American Board of Urology. His clinical special interests include: kidney stone disease, urinary incontinence, benign prostatic hyperplasia, prostate cancer, and surgical oncology. He lives in Wenatchee, WA and enjoys hunting, fishing, hiking, and spending time with his wife Laura and their three children.
 Mary Kathryn Resk cannot sit idle for long. As a result, she is a teacher, freelance writer, performer, traveler, athlete, and community volunteer who lives on the foothills of the Cascades in central Washington state. She was thrilled to make her first trip to Milot, Haiti this spring alongside her anesthesiologist husband, Dr. John Rompala. For more on her current projects and escapades, visit: http://www.mkresk.wordpress.com
Mary Kathryn Resk cannot sit idle for long. As a result, she is a teacher, freelance writer, performer, traveler, athlete, and community volunteer who lives on the foothills of the Cascades in central Washington state. She was thrilled to make her first trip to Milot, Haiti this spring alongside her anesthesiologist husband, Dr. John Rompala. For more on her current projects and escapades, visit: http://www.mkresk.wordpress.com









